Share Post
Introduction
A bunion can start as a small, barely noticeable bump and gradually become a source of daily discomfort. If you’ve noticed your big toe drifting toward your second toe or struggling to find comfortable shoes, you’re not alone. This guide covers everything from simple home remedies to surgical options, helping you understand when each approach makes sense for your situation.
What Is a Bunion?
A bunion is a visible bump that forms at the joint at the base of your big toe—the first metatarsophalangeal joint, or MTP joint. It’s not simply “extra bone” growing on your foot. Rather, it’s a combination of bone misalignment, joint enlargement, and sometimes swollen tissue on the inner side of your foot.
The medical term for this condition is hallux valgus, which describes exactly what happens: your big toe points inward toward your other toes while the metatarsal bone drifts outward, creating that characteristic bony bump on the side of your foot.
Bunions are progressive deformities, meaning most bunions worsen gradually over years. They tend to accelerate in adults during their 40s, 50s, and beyond due to cumulative mechanical stress. Statistics show that up to 23% of adults over 18 and 35.7% of those over 65 have bunions, with women affected three times more often than men.
On physical examination, bunions typically appear as a red, swollen bump with the big toe angling toward the little toe side of the foot. In moderate to severe cases, the toe may crowd or overlap the second toe.
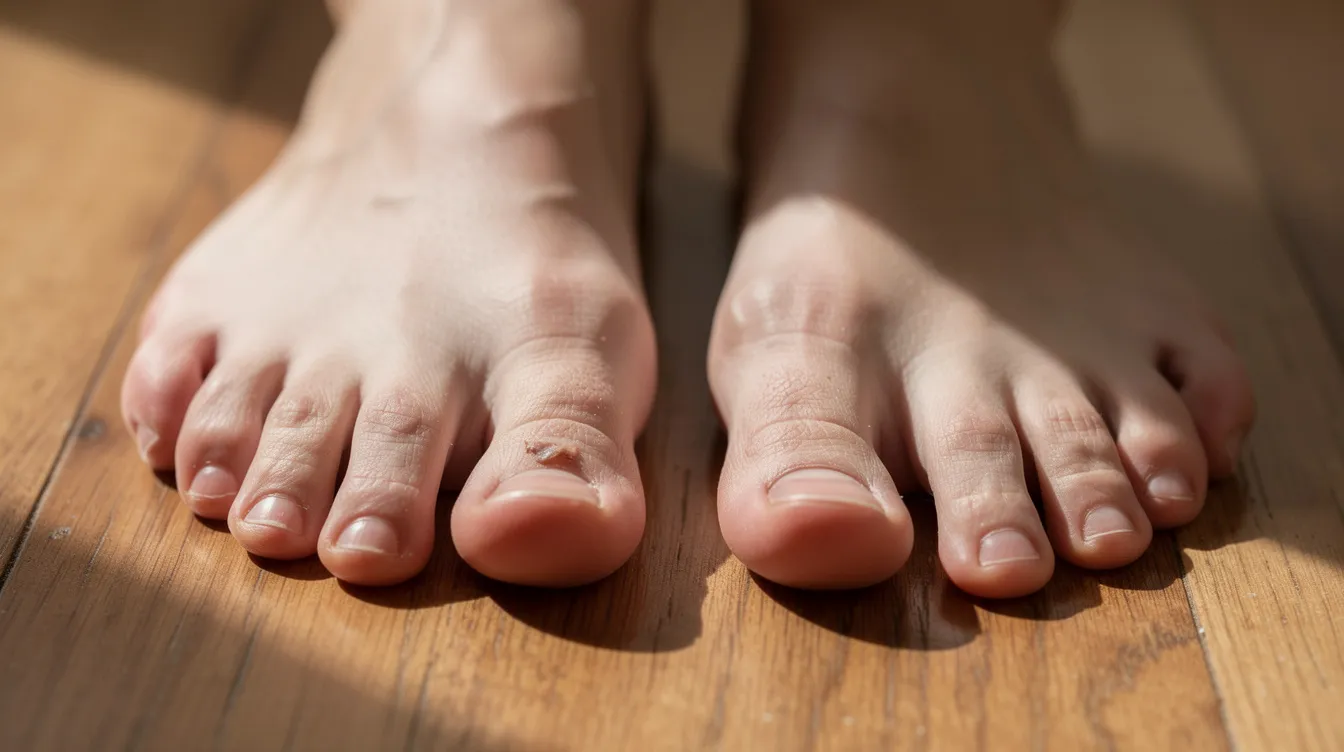
Common Symptoms of a Bunion
Not all bunions cause problems. Some people have only mild cosmetic concern, while others experience bunion symptoms that are extremely painful and limit walking or shoe choices.
Common signs include:
- A bony bump at the base of the big toe
- Soreness or aching after walking or standing
- Redness and pain and swelling over the bump
- Stiffness in the big toe joint, reducing range of motion by 20-50%
Tight or narrow shoes, high heels, and prolonged standing make symptoms worse by increasing constant pressure on the toe joint. Research shows high heeled shoes shift up to 75% of body weight forward, dramatically amplifying stress on the MTP joint.
Associated foot problems include:
- Calluses or corns on adjacent toes
- Ingrown toenails from crowding
- Difficulty finding well fitting shoes
- Gait changes that may lead to knee or hip strain
Symptoms often fluctuate day to day, with flare-ups after long walks, runs, or events where dress shoes are worn for hours.
What Causes Bunions?
Bunions form from a combination of inherited foot structure and long-term mechanical stress. You can blame your parents for some of it—genetics account for 44-69% of bunion risk according to twin studies.
Inherited factors that predispose you to bunions:
- Flat feet or low arches
- Hypermobile joints or loose connective tissue
- Abnormal bone structure, particularly a long first metatarsal
External factors that accelerate progression:
- Wearing narrow shoes or high heels regularly
- Wearing shoes that are too tight or loose
- Occupations requiring prolonged standing (nurses show 2x higher rates)
- Inflammatory conditions like rheumatoid arthritis (up to 90% develop bunions)
- Previous foot injuries
Shoes alone rarely cause a bunion in someone with neutral foot mechanics, but they can accelerate progression by 1-2 degrees per year in those with underlying structural risk.
Can Bunions Be Reversed?
Here’s the straightforward answer: once a bunion has formed, it does not go away on its own. No exercise, toe spacers, or night splint can fully reverse the bone alignment in adults.
Non-surgical treatments focus entirely on symptom control—reducing pain and swelling—and slowing progression. They do not permanently straighten the bone.
Toe spacers and night splints can temporarily improve toe position by 3-5 degrees during wear, providing comfort. However, once removed, the toe returns to its misaligned position. These devices work through soft tissue stretch, not bone remodeling.
The only way to fix bunions permanently and realign the affected toe to its correct position is through surgery. However, this doesn’t mean everyone needs an operation. Many people (70-80% with mild-moderate bunions) manage comfortably their entire lives with conservative treatment alone.
Home and Non-Surgical Bunion Treatments
Non-surgical care is always the first step for treating bunions. Most interventions can be started at home, often with guidance from a foot doctor or family physician.
Pain Relief Options
Over the counter medicines:
- NSAIDs like ibuprofen (400-600mg every 6-8 hours) or naproxen help reduce inflammation
- Use short-term only (under 2 weeks) to avoid kidney or GI issues
- Avoid if you take blood thinners or have ulcer history
Any pain reliever should be used as directed and discussed with your healthcare provider.
Temperature Therapy
Cold therapy: Apply an ice pack wrapped in a thin towel to the bunion for 10-15 minutes after activity. This can reduce swelling by 30-50% and relieve pain effectively. Never apply ice directly to bare skin.
Heat therapy: Warm soaks or a heating pad on low setting relaxes surrounding muscles and eases stiffness before gentle stretching. This improves blood flow to the area.
Activity Modifications
- Take shorter walks during flare-ups
- Avoid running on hard pavement
- Choose low-impact exercise: swimming reduces forefoot load by 90% compared to running
- Cycling and elliptical training are excellent alternatives
Weight and Exercise
Maintaining a healthy weight reduces stress on your forefoot. Even a 5-10 kg weight loss can noticeably decrease daily foot pressure (10-15 mmHg reduction per studies).
Simple toe exercises for mobility:
- Towel scrunches (3 sets of 10 reps daily)
- Picking up marbles with your toes
- Toe curls and spreads
These exercises maintain strength and flexibility but are for symptom control, not deformity reversal.
Treating Bunions With Footwear and Orthotics
Shoe choice is one of the most powerful everyday tools for bunion pain relief. Wearing shoes with proper fit can eliminate pain during daily activities and significantly slow progression.
Ideal Bunion-Friendly Shoes
| Feature | What to Look For |
|---|---|
| Toe box | Wide and deep toe boxes (1-1.5cm wider than foot) |
| Upper material | Soft, flexible over the bunion area |
| Heel counter | Firm for stability |
| Arch support | Built-in or compatible with shoe inserts |
| Heel height | Under 2-3cm |
Try shoes late in the day when feet are slightly swollen (5-10% larger) to ensure adequate space. Get professionally measured for both length and width.
Padding and Spacers
- Bunion pads (gel or felt) placed over the bump reduce friction by 50-70%
- Toe spacers between the big toe and second toe relieve pressure and crowding
- Both are for comfort only—they don’t change bone position
Orthotic Devices
- Drugstore insoles work for mild cases
- Custom-made orthotics prescribed by our podiatrists help with flat feet or overpronation
- Custom orthotics can redistribute 20-30% of medial pressure, slowing progression 15-25% over two years
Footwear changes and orthotics do not shrink bunions but can significantly reduce pain and make daily walking comfortable. The American Podiatric Medical Association recommends supportive shoes as foundational care.

Medical and Surgical Bunion Treatment Options
When home care isn’t enough—persistent pain despite good shoes, difficulty walking normal distances, or rapid worsening—it’s time to see a specialist.
Medical Evaluation
Your foot doctor will perform:
- Complete foot examination
- Review of symptoms and current footwear
- Weight-bearing X-rays measuring the intermetatarsal angle (normal is under 8 degrees) and checking for an arthritic bunion
In-Office Treatments
- Prescription-strength anti-inflammatories
- Corticosteroid injections for severe inflammation (4-6 week relief)
- Referral to physical therapy for targeted exercises and gait training
Surgical Options
Bunion surgery aims to realign one or more bones, correct the deformity, and relieve pain—not just shave off the bump.
Types of bunion surgery:
| Severity | Procedure | Description |
|---|---|---|
| Mild | Exostectomy + soft tissue balancing | Shaving the bump and rebalancing ligaments |
| Moderate | Osteotomy (Chevron/Austin) | Cutting and repositioning the metatarsal with screws/plates |
| Severe bunion | Lapidus Bunion Procedure | Fusion for severe arthritis |
| Any | Minimally invasive (MIS) | 3 small incisions, less scarring, faster recovery |
Recovery Expectations
- Walking in a protective boot: few days to 2 weeks
- Swelling persists: 3-6 months
- Return to most activities: 8-12 weeks
- High-impact sports: often delayed longer
Surgery achieves 85-90% satisfaction rates for pain relief. However, decisions should be based on pain and function, not appearance alone. A detailed discussion with ankle surgeons or orthopedic specialists is essential.
Blood tests may be ordered pre-surgery to check for conditions affecting healing.

Preventing Bunions and Slowing Their Progression
You cannot change inherited foot structure, but you can influence how quickly bunions form or worsen.
Key prevention strategies:
- Consistent footwear choices: Wear supportive shoes with deep toe boxes daily. Reserve narrow or high-heeled shoes only for short, occasional use—this alone can limit progression by 20-30%.
- Weight management: Balanced diet and regular low-impact exercise keep forefoot pressure low. Remember: 10kg loss equals about 4kg less pressure per step.
- Daily stretching: Calf and Achilles stretches (30-second holds, 3 repetitions) maintain 10-15% flexibility gains and reduce strain on the big toe joint.
- Early monitoring: Inspect your feet regularly for early signs—slight drift of the big toe, mild redness at the inner joint. Seek professional advice early rather than waiting until pain becomes extreme pain.
- Proactive care for high-risk individuals: Those with flat feet, hypermobility, or strong family history benefit from early orthotic use and periodic podiatry checkups.
To prevent bunions from worsening, avoid wearing narrow or pointed shoes regularly.
Living With a Bunion: Outlook and Quality of Life
Many people live active, comfortable lives with bunions by combining the right shoes, home care, and periodic medical follow-up. About 60-70% maintain excellent quality of life through multimodal care.
However, untreated or poorly managed bunions can:
- Cause chronic pain limiting walking to under 1km
- Lead to 40% sports dropout rates
- Create frustration with limited shoe options
Early and consistent conservative management often prevents these limitations. Work with your healthcare provider to set realistic goals—being able to walk a certain distance without pain, stand through a work shift, or attend events comfortably.
View bunion management as an ongoing process. Your treatment plan may need adjustments over time: new orthotics, different shoes, or eventually considering surgery if daily life remains restricted.
Key Takeaways
- Bunions are progressive deformities at the base of the big toe that typically worsen over time, but early non-surgical bunion treatment can significantly reduce pain and slow progression.
- First-line treatments include comfortable shoes with a wide toe box, orthotic devices, bunion pads, and simple home measures like nonsteroidal anti inflammatory drugs and ice packs.
- No exercise, splint, or shoe can reverse a bunion completely—only bunion surgery can permanently correct the bony deformity and realign the affected joint.
- Most bunions (over 80%) are managed successfully without surgery, but severe pain or major deformity warrants consultation with foot and ankle surgeons.
- Modern surgical techniques in 2025-2026 allow weight-bearing within days, with many patients returning to normal activities in 8-12 weeks and full recovery in up to six months.
FAQ’s
Do bunion correctors and night splints really work?
Bunion correctors, sleeves, and night splints can improve comfort by reducing pressure and gently holding the affected toe in a straighter normal position while resting. In adults, they do not permanently change bone alignment—studies show no significant radiographic change. However, they may reduce pain by 20-40%, prevent rubbing inside shoes, and help some people sleep better. Treat them as part of a comfort strategy alongside good shoes and orthotics, not as a cure.
Is it safe to keep running or playing sports if I have a bunion?
Many people continue to run and play sports with bunions if pain is controlled and footwear is appropriate. Switch to wider athletic shoes, use padding over the bunion, and choose surfaces and training volumes that don’t trigger major flare-ups. However, if you experience sharp pain, sudden worsening of deformity, or difficulty bearing weight, pause high-impact activity and seek evaluation. Swimming and cycling are excellent alternatives during recovery periods.
Can children and teenagers develop bunions, and should they be treated differently?
Yes, bunions can begin in childhood or adolescence (juvenile hallux valgus), representing 10-15% of pediatric podiatry visits. These cases are more common in those with strong family history or flat feet. Treatment focuses on supportive footwear, orthotics, and close monitoring of growth. Surgery is rare (under 5% of cases) and generally reserved for severe, painful deformities that continue to worsen. Parents should have a pediatric podiatrist assess any noticeable big toe drift or bump early.
Will wearing high heels occasionally ruin my bunion treatment progress?
Occasional short-term wear of high heels for special events is usually acceptable if day-to-day shoes are bunion-friendly and symptoms are mild. Focus on moderation: lower heel height, wider toe box dress shoes, and bringing a more supportive pair to change into when possible. Those with severe pain, recent bunion surgery, or a tailor’s bunion should avoid high heels until cleared by their surgeon. Limit wear to under 4 hours when possible.
How do I know if my bunion is severe enough to need surgery?
Severity is judged by both X-ray measurements and functional impact.
Strong indicators for surgery include:
Persistent pain despite 3-6 months of good conservative treatment
Pain above 4/10 that limits daily activities
Significant difficulty fitting into normal shoes
Progressive deformity with overlapping toes
Intermetatarsal angle over 8 degrees on X-ray1
If uncertain, book a consultation with foot and ankle surgeons. They’ll review imaging, discuss risks and benefits, and help you decide on timing together.
Contact Form – Calgary Podiatry
Contact Form – Please let us know about your condition in the below box so our team can better assist you.